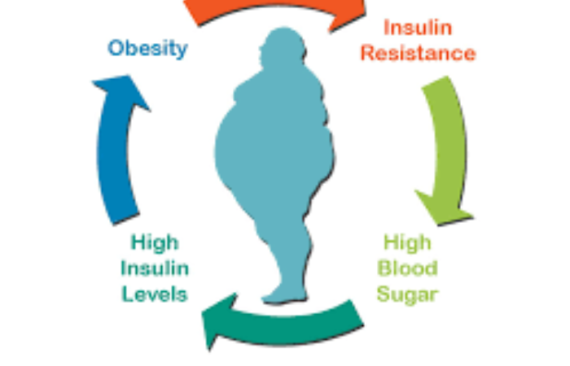
Obesity and diabetes are closely linked, and the relationship between the two is complex. While obesity doesn’t directly cause diabetes, it is a significant risk factor for developing type 2 diabetes, which is the most common form of diabetes. Here’s how obesity contributes to diabetes and how weight loss can have a positive impact:
- Insulin Resistance: In type 2 diabetes, there is a condition called insulin resistance, where the body’s cells become less responsive to the effects of insulin, a hormone that helps regulate blood sugar (glucose) levels. Obesity is associated with chronic low-grade inflammation and the accumulation of fat in certain tissues, particularly in and around organs like the liver and muscles. This can disrupt the normal functioning of insulin signaling pathways and lead to insulin resistance.
- Adipose Tissue Dysfunction: Adipose tissue, or fat tissue, is not just a passive storage site for energy; it’s also an active endocrine organ that produces various hormones and molecules. In obesity, there is an increased release of certain substances like free fatty acids and inflammatory cytokines from adipose tissue. These substances can interfere with insulin signaling, further promoting insulin resistance and contributing to the development of diabetes.
- Pancreatic Strain: The pancreas is responsible for producing insulin. In obesity, the increased demand for insulin due to insulin resistance can put a strain on the pancreas. Over time, the pancreas might struggle to produce enough insulin to maintain normal blood sugar levels, leading to the development of diabetes.
- Metabolic Syndrome: Obesity often occurs alongside other metabolic abnormalities, such as high blood pressure, high cholesterol levels, and abnormal lipid profiles. These factors collectively contribute to a condition called metabolic syndrome, which increases the risk of diabetes and cardiovascular diseases.
Weight loss can play a significant role in managing and, in some cases, even reversing type 2 diabetes. When an individual with obesity loses weight, several positive changes occur:
- Improved Insulin Sensitivity: Weight loss can lead to a reduction in fat accumulation in tissues, especially in the liver and muscles. This can help restore insulin sensitivity, making the cells more responsive to insulin’s actions.
- Reduced Inflammation: Losing weight can lead to a decrease in the release of inflammatory molecules from adipose tissue. This reduction in chronic inflammation can have a positive impact on insulin signaling and overall metabolic health.
- Lowered Pancreatic Strain: With weight loss and improved insulin sensitivity, the demand on the pancreas to produce insulin is reduced. This can help preserve pancreatic function and prevent further deterioration.
- Better Management of Blood Sugar: As insulin sensitivity improves and the body becomes more responsive to insulin, blood sugar levels tend to stabilize, reducing the need for diabetes medications and improving overall glycemic control.
It’s important to note that while weight loss can greatly improve the management of type 2 diabetes, it might not be a cure for everyone. Genetics, underlying metabolic factors, and the duration of diabetes can influence the extent to which weight loss can reverse the condition. Additionally, maintaining a healthy lifestyle, including regular physical activity and a balanced diet, is crucial for long-term diabetes management and overall well-being. If you’ve been diagnosed with Type 2 diabetes and are overweight, our weight loss solutions may offer you a path to a new, healthier life free from obesity and diabetes. We invite you to contact us today to get started.